This guide explains how to use a patient's Account Enquiry screen to review, investigate, adjust and receipt invoices, and the different indicators available.
Overview
The Account Enquiry screen is used to administer invoices without claims and to update claims and payments that cannot be managed in Zedmed's Claims and Payments screens. This is explained in table below, which links specific tasks to the relevant process.
To access the Account Enquiry screen:
- Open the patient's record.
- Select the Acc Enquiry menu.
The Account Enquiry screen will open.

Top menu
The following options are available on the top menu:
- Payer - view just the invoices for the payer selected in the drop-down box.
- Recalculate recalculates the Outstanding amounts when you select a payer; generally, this is done automatically.
- Display Invoices - select the invoice status you want to view. Acc Enquiry shows outstanding invoices by default.
- Full Details - expand the invoices and display each line item and any credits or outstanding amounts for the payer.
- Allocation - allocate credits to outstanding invoices. Button is selectable if there is an Account Payer Credit for that Payer.
Invoice notes
Add a note to an invoice. This is useful when following up with patients on unpaid invoices or turning a quote into an invoice.
To add a note:
- Open the patient's record and select Acct Enquiry.
- Select the invoice.
- Select the Edit Note button
The Invoice Note Editor will open. - Type the text
- Select Close to save.
These steps can also beused to edit a note.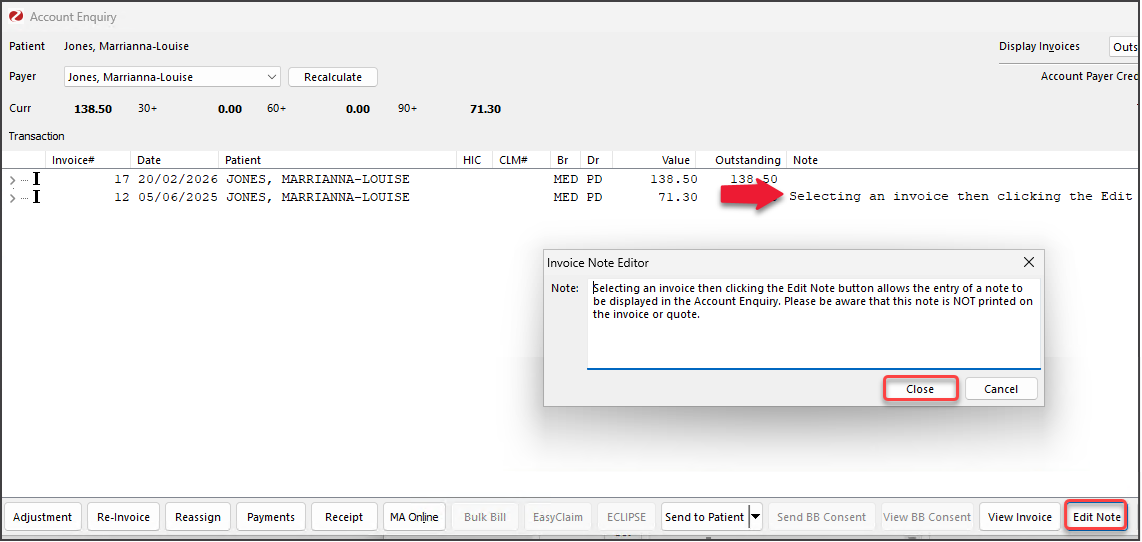
Invoice codes
Each invoice's component/status is indicated as follows:
- I:Invoice. Displays invoice number, creation date, branch and the doctor is was billed under.
- S: Service item. Displays date of service, item billed, who billed it and amount of item.
- R: Receipt. Displays date of receipt, receipt number and who receipted it.
- A: Adjustment. Displays any adjustments made to the invoice.
- Green tick. Indicates that the invoice or service item as been receipted.
- Red cross. Indicates that the invoice or service item has been voided.
- N: Note. Displays any notes that were added to the invoice when creating it.
- Q: Quote. The invoice is a quote for the patient.
HIC column codes:
- E: Eclipse. The invoice has been transmitted to ECLIPSE.
- R: Real-time assessed. Indicates the patient's claim has been sent to Medicare.
Account Enquiry buttons
The buttons along the bottom of the Acc Enquiry screen:
- Adjustments - for making billing adjustments, including Medicare Same Day Delete and Voiding. Each type is explained below.
- Re-Invoice - Allows you to make changes to an invoice without completely voiding & re-billing.
- Reassign - Assign an invoice from one payer to another.
- Payments - Displays past payments receipted against that payer.
- Receipt - Receipt a new payment.
The payer options shown will depend on the patient's default payer. - MA Online - Transmit the patient's claim to Medicare.
- Eclipse - Transmit the patient's claim to Eclipse.
- Bulk Bill - Transmit the patient's claim to Medicare.
- DVA - Transmit the patient's claim to the DVA.
- Send to Patient - has 2 options: Secure Send or email the selected invoice to the patient.
- EasyClaim - instantly process an invoice that has a claimable contribution to a patient's Debit card.
- View Claim/Invoice - Display the invoice or rebate details. You can print from the display screen.
- Print - Prints the selected invoice.
- Email Statement - Emails an Activity Statement of all invoices that include the Status, Date and amount.
- Close - Exit Account Enquiry.
Actions performed in Acc Enquiry
Tasks for private patients and thirty-party payers, and some claim-related tasks, are managed in the Account Enquiry screen.
| Action | Where to perform the action | Important information - read before performing the action |
| Void a Medicare invoice you just created if you call Medicare the same day. Read Notes section-> | Select Invoice > Adjustment >Void every service in the Adjustment screen. | Warning: Medicare does not know when an invoice is voided and will pay it, so you MUST call them to stop payment on the SAME day you void the invoice to avoid reconciliation errors. |
| Amend an invoice (Reinvoice). | Select Invoice > Reinvoice > Make the required changes to the invoice. | If you have an invoice with no claim ID (e.g. a claim was suppressed) you can amend the invoice using this option. Reinvoicing will automatically Void the original invoice.
This option will not work on a receipted invoice. In this scenario, you would void the invoice and create a replacement. |
| Submit a claim for a suppressed invoice. | Select Invoice > Select Payer (e.g. Bulk Bill) | You can transmit suppressed invoices one at a time from the Acc Inquiry screen or in bulk from the Claims tab. |
| Void a MA Online invoice. | Select Invoice > Adjustment > MA Same Day delete. | When the rebate submitted for the patient, you can use this process to void the invoice and stop the payment. |
| Manually adjust an invoice that cannot be auto-adjusted in the Payment tab. | Select Invoice > Patient or 3rd Party Adjustment > Select the Service row then Discount or Increase or Void. | If a Payment ID with multiple claims includes a voided invoice, all invoices covered by that Payment ID must be manually adjusted. |
| Provide rebate details for the patient. | Select Invoice > View Claim > Print the report when it opens. | This report shows the rebate amount to the patient. |
| Manage payments by patients who paid their own bill. | Receipt payments for deferred bills.
Adjust an invoice for a private patient Refund a payment to a private patient |
Patients who pay their own bills do not generate claims, so receipting, refunds and adjustments are all managed in the patient's Acc Enquiry. |
| Manage payments by a 3rd party for a patient. | Refund a payment to a 3rd party.
Adjust an invoice paid by a 3rd party. Receipt a payment by a 3rd party. |
Patients whose bills are paid by an employer or organisation, like the TAC, do not generate Medicare claims, so receipting, refunds and adjustments are all managed in Acc Enquiry. |
Tasks often performed in the Claims Screen
| Task | Where to perform the action | Important information - read before performing the action |
| Void a rejected item in an invoice. | Management > Claims > Payments tab > Reconcile Payment - Tick Void Rejected Services. | You void items Medicare rejected so the invoice can be reconciled. You may want to check the Claims tab to see the reason and possibly raise a revised invoice (claim) for the item. |
| Void a rejected invoice. | Management > Claims > Claims tab > Select Status REJECTED invoices > Void Rejected Invoices. | On a regular basis, you should use the REJECTED filter to show all rejected invoices, review the reason for possible reinvoicing, then void the rejected invoices. |
| Adjust invoices for under and overpayments. | Management > Claims > Payments tab > Reconcile Payment - Under and overpayment adjustment ticked by default. | The adjustments are made automatically, so no manual adjustments are required. You can review the reason for reinvoicing but it will often be an out-of-date fees file. |

